When facing a prostate cancer diagnosis, many men find themselves weighing the choice between open and robotic-assisted prostatectomy. Both are established surgical methods for removing the prostate gland, yet the technology, recovery time, and long-term outcomes can vary. Recent studies and growing clinical experience have fuelled a lively debate about which option is best. This article aims to provide clarity, explaining what the evidence really shows, and how your surgical choice might affect your recovery, cancer control, and quality of life.
What the research says about open vs robotic surgery
Clinical trials and large-scale studies have tried to settle the debate between open prostatectomy and robotic-assisted techniques. One of the most frequently cited studies, a 2016 randomised trial published in The Lancet, found similar cancer control outcomes at the two-year mark between the two techniques. However, this study has notable limitations. The surgeons involved had limited robotic experience, and patients did not benefit from newer advances like Retzius-sparing approaches or intraoperative nerve testing, such as the NeuroSAFE technique.
In reality, the success of prostate cancer surgery is not defined by the robot, or the lack of one, but by the surgeon operating it. Robotic systems, including the da Vinci Single Port platform, offer remarkable tools for fine dissection and nerve preservation, but these benefits only translate into better outcomes when used by highly skilled hands.
Further analysis of the Lancet study reveals that patients undergoing open surgery experienced three times more blood loss, higher complication rates, and greater pain one week post-operation compared to those who had robotic surgery. Moreover, the open surgery group reported a worse quality of life at six weeks post-surgery. It’s also noteworthy that the open surgeon had 15 years of experience, while the robotic surgeon had only two years, suggesting that with equal experience, robotic surgery might offer even more pronounced benefits.
At Santis Health, we have performed over 4,000 keyhole prostatectomies, making us one of the most experienced minimal access surgery teams in the UK. Our extensive experience with robotic-assisted procedures, combined with advanced techniques like Retzius-sparing and NeuroSAFE, positions us at the forefront of prostate cancer surgery, aiming to provide optimal outcomes for our patients.
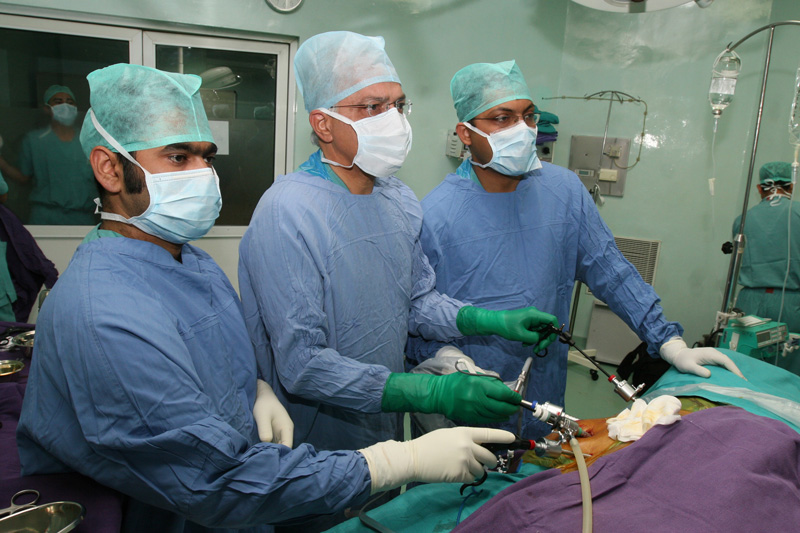
Differences between open and robotic prostatectomy
While both surgeries aim to remove the prostate and surrounding tissues affected by cancer, their approach, precision, and recovery experience differ substantially. Robotic-assisted prostatectomy is a form of minimally invasive surgery performed through a few small incisions using advanced robotic instruments. In contrast, open radical prostatectomy involves a single, larger incision through the lower abdomen, with surgeons working directly on the tissues.
Robotic systems offer a 10× magnified 3D view of the operating field, translating the surgeon’s hand movements into precise micro-motions. This allows for better visualisation of nerves and vessels, which can lead to improved functional outcomes like continence and sexual function. Open surgery, while reliable and familiar to many clinicians, provides a more limited view as the prostate is located deep in the pelvis and often results in greater blood loss and longer recovery times.
| Feature | Open Prostatectomy | Robotic Prostatectomy |
|---|---|---|
| Invasiveness | Large incision (8–10 cm) | Small incisions (1–2 cm) |
| Blood Loss | Higher; often >500ml | Lower; often <200ml |
| Complication Risk | Higher infection & pain risk | Lower complication rates overall |
| Recovery Time | 4–6 weeks off work | 1–2 weeks off work |
| Margin Positivity | Depends on surgeon skill | Often lower in expert hands |
Feature: Invasiveness
Open Prostatectomy : Large incision (8–10 cm)
Robotic Prostatectomy : Small incisions (1–2 cm)
Feature: Blood Loss
Open Prostatectomy : Higher; often >500ml
Robotic Prostatectomy : Lower; often <200ml
Feature: Complication Risk
Open Prostatectomy : Higher infection & pain risk
Robotic Prostatectomy : Lower complication rates overall
Feature: Recovery Time
Open Prostatectomy : 4–6 weeks off work
Robotic Prostatectomy : 1–2 weeks off work
Feature: Margin Positivity
Open Prostatectomy : Depends on surgeon skill
Robotic Prostatectomy : Often lower in expert hands
Recovery and functional outcomes
Continence
One of the most concerning post-operative side effects for men undergoing prostatectomy is urinary incontinence. Robotic-assisted surgery, especially when performed with the Retzius-sparing approach, has been shown to significantly shorten the time to continence recovery. This method avoids disrupting the structures in front of the bladder, which play a key role in urinary control. Many patients at Santis regain continence within weeks, whereas traditional open surgery may take several months.
Recent data from over 400 cases at Santis Health indicates that 90% of men who undergo Retzius-sparing robotic prostatectomy are immediately continent upon catheter removal, while also experiencing significantly better post-surgery potency, all with no negative impact on cancer control. Furthermore, at four weeks post-surgery, 90% of men used 0 pads per day, and 97.5% used 0–1 pads per day.
Erectile function
Preserving erectile function after surgery hinges on two key factors: whether the cancer has spared the nerves, and whether those nerves can be safely preserved during the operation. Robotic surgery enhances the chances of preserving the neurovascular bundles due to better visualisation and refined dissection. In some cases, intraoperative nerve-monitoring systems such as NeuroSAFE are used to assess margins in real time, allowing for more confident nerve-sparing. Recovery of erections can still take time, up to 3 years, but men who undergo robotic prostatectomy with nerve-sparing techniques tend to report better outcomes.
Recent data from Santis Health indicates that patients who undergo nerve-sparing robotic prostatectomy experience a higher rate of erectile function recovery. Specifically, studies have shown that a significant percentage of men regain satisfactory erectile function within 12 months post-surgery. These outcomes are attributed to advanced surgical techniques and the use of intraoperative nerve monitoring, which collectively enhance the preservation of erectile nerves during the procedure.
Return to normal activities
Robotic-assisted surgery also enables a quicker return to daily routines. Many patients leave hospital the morning after their operation, and are back to desk-based work within 10–14 days. Driving, light walking, and socialising can resume within days, while more strenuous activity may take four to six weeks. In contrast, open surgery patients usually face a longer hospital stay and recovery period, with more post-operative discomfort.
The use of the da Vinci Single Port (SP) robotic system has further enhanced recovery outcomes. This advanced technology allows for all surgical instruments to be inserted through a single small incision, reducing post-surgery discomfort and accelerating recovery times. Patients undergoing procedures with the SP system often experience less pain, minimal scarring, and a faster return to normal activities compared to traditional multi-port robotic surgery.
Moreover, the integration of techniques like the Retzius-sparing approach has significantly improved functional outcomes. It bears repeating that recent data from Santis Health indicates that 90% of men who undergo Retzius-sparing robotic prostatectomy are immediately continent upon catheter removal, and 97.5% use 0–1 pads per day at four weeks post-surgery. These advancements collectively contribute to a more comfortable and swift recovery process for patients.
Recovery timeline: Returning to normal after robotic prostatectomy
Day 0–1: Surgery and overnight hospital stay. Patients are usually up and walking the next morning.
Day 2: Discharged home with catheter in place; encouraged to walk for 30 minutes each day.
Week 2: Catheter typically removed. Most men have reasonable urinary continence immediately.
Weeks 3–4: Many return to desk-based work and light activity. Pad use for minor leaks may still be needed.
Weeks 6–12: Physical activity increases. Significant gains in continence and potency, especially with nerve-sparing.
Months 3–12: Ongoing improvements in urinary and sexual function, monitored through regular follow-ups and PSA testing.
When is robotic prostatectomy typically recommended?
Robotic-assisted prostatectomy is often the preferred option for patients with localised prostate cancer who wish to preserve urinary and sexual function, and who are medically fit for surgery. Younger men, in particular, benefit from the quicker return to baseline function and the ability to resume their personal and professional lives sooner.
Tumour location also plays a part. When the cancer is close to nerves or confined to the front of the prostate, the enhanced precision of robotic instruments can make nerve-sparing and complete tumour removal more feasible. At Santis, we specialise in these complex cases, often using the da Vinci Single Port system and Retzius-sparing approach for optimal results.
Robotic surgery is also a strong choice for men seeking to preserve future treatment options. Unlike radiotherapy, which may complicate later surgery due to tissue changes, robotic surgery keeps the door open for additional therapies if needed. It also eliminates the small but real risk of secondary cancers associated with radiation exposure.
Choosing the right surgery for you
While both open and robotic-assisted prostatectomy can be effective for managing prostate cancer, the robotic approach offers compelling advantages in terms of precision, recovery speed, and functional preservation, particularly in the hands of experienced surgeons. At Santis Health, we bring unparalleled expertise and cutting-edge technology to every procedure, ensuring that patients receive not just treatment but a greater probability of the best possible outcome.
If you’re navigating your prostate cancer treatment options and want guidance tailored to your needs, book a consultation with our team today. We’re here to help you make the best possible decision for your future.

